Opiate Withdrawal
Summary
The use and abuse of opioids can be traced back to ancient cultures. Awareness of the pain relieving and euphoric effects of opioids is evident within Sumerian culture dating back to 4000 BC.
According to Adrian Preda, M.D., Professor of Psychiatry and Human Behavior at the University of California Irvine School of Medicine, opioids can be divided into three classes:
Opiate Withdrawal
- Naturally occurring opioids: The classic natural opioids are opium and morphine. Opium is extracted from the plant Papaver somniferum (the opium poppy), and morphine is the primary active component of opium. Endogenous neural polypeptides such and endorphins and enkephalins are also natural opioids.
- Semi-synthetic opioids: Semisynthesis is a type of chemical synthesis that uses compounds isolated from natural sources (eg, plants) as starting materials. Semi-synthetic opioids include heroin, oxycodone, oxymorphone, and hydrocodone.
- Synthetic opioids: Synthetic opioids are made using total synthesis, in which large molecules are synthesized from a stepwise combination of small and cheap (petrochemical) building blocks. Synthetic opioids include buprenorphine, methadone, fentanyl, alfentanil, levorphanol, meperidine, codeine, and propoxyphene (withdrawn from US market).
These three classifications are determined “by their ability to bind to and influence opiate receptors on cell membranes” (Preda).
A Brief History
Opioid abuse and addiction experienced global awareness beginning in the early 20th century. In 1909, to help China battle its opium smoking predicament, U.S. President Theodore Roosevelt convened the Shanghai Opium Commission.
Important milestones throughout the 20th century concerning opioid abuse and dependence include: the Harrison Narcotics Tax Act of 1917 outlawed the use of opioids as treatment for opioid addiction; the Methadone Maintenance Research Program, directed by Drs. Dole and Nyswander during the mid-1960s, determined methadone to be an effective alternative to heroin in the treatment of addicts; in 1974, the Narcotic Addict Treatment Act “allowed regulated methadone treatment for opioid addiction, but made off-label use of opioids illegal”; in 2000, the Drug Addiction Treatment Act allowed qualified physicians to prescribe buprenorphine as a replacement treatment strategy for opioid addiction (Preda).
Opioid Dependence
Opioids are widely accepted as the foremost weapon against severe, chronic pain – but physicians are currently forced to weigh the risk of abuse and misuse of prescription opioids versus the benefits on a case by case basis.
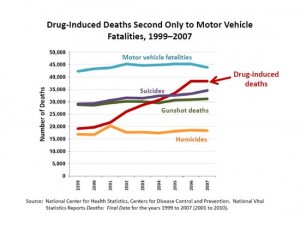
The rise in overdose deaths among those prescribed opioids for control of pain have led to sanctions against physicians and have become an important variable in pain management. Among the risks associated with opioid abuse and misuse are:
- Overdoses
- Addiction and dependence
- Adverse effects
- Social and family dysfunction
- Criminal consequences (“Use, Abuse”)
Figures from the American College of Preventive Medicine clearly illustrate the risk of opioid abuse among pain patients:
Opioids are the most abused drugs in the chronic pain setting. The prevalence of lifetime substance use disorders ranges from 36% to 56% in patients treated with opioids for chronic back pain; 43% of this population has current substance use disorder (SUD) and 5% to 24% have aberrant medication-taking behaviors. About 14% to 16% of pain patients not having SUD use illicit drugs in combination with prescription drugs for pain, while 34% of patients with SUD combine legal pain medication with illicit drug use. These statistics highlight the difficult situation of balancing pain treatment with abuse management. Studies show that increased monitoring of these situations does indeed decrease controlled substance abuse and illicit drug use (qtd in “Use, Abuse”).
Opioid Withdrawal
Having developed a physical and psychological dependence upon opioids, if the individual is to attempt to discontinue use of opioids, one must first endure withdrawal symptoms which can range from uncomfortable to agonizing.
Buprenorphine – a semi-synthetic opioid- is often administered by physicians to aide detoxification and to ease withdrawal symptoms. Early withdrawal symptoms include:
- Agitation
- Anxiety
- Muscle aches
- Increased tearing
- Insomnia
- Runny nose
- Sweating
- Yawning
Later symptoms include:
- Abdominal cramping
- Diarrhea
- Dilated pupils
- Goose bumps
- Nausea
- Vomiting
“Opioid withdrawal reactions are very uncomfortable but are not life threatening. Symptoms usually start within 12 hours of last [opioid] usage…” (“Opiate Withdrawal”).
While rarely life threatening, professionally guided detoxification is urged as many complications may arise during withdrawal. The National Institutes of Health (NIH) lists the following risks associated with opioid withdrawal:
Complications include vomiting and breathing in stomach contents into the lungs. This is called aspiration, and can cause lung infection. Vomiting and diarrhea can cause dehydration and body chemical and mineral (electrolyte) disturbances.
The biggest complication is return to drug use. Most opiate overdose deaths occur in people who have just withdrawn or detoxed. Because withdrawal reduces your tolerance to the drug, those who have just gone through withdrawal can overdose on a much smaller dose than they used to take.
Long Term Treatment
Longer-term treatment is recommended for most people following withdrawal. This can include self-help groups, like Narcotics Anonymous or SMART Recovery, outpatient counseling, intensive outpatient treatment (day hospitalization), or inpatient treatment.
Those withdrawing from opiates should be checked for depression and other mental illnesses. Appropriate treatment of such disorders can reduce the risk of relapse. Antidepressant medications should NOT be withheld under the assumption that the depression is only related to withdrawal, and not a pre-existing condition.
Treatment goals should be discussed with the patient and recommendations for care made accordingly. If a person continues to withdraw repeatedly, methadone maintenance is strongly recommended (“Opiate Withdrawal”).
Based upon research which shows that, despite proper detoxification from opioids, relapse is common. Continued treatment following the detox process is highly encouraged. Recent studies involving animals appears to identify three conditions which are predictors to relapse:
- Stress
- Exposure to conditioned cues related to past drug use
- A dose of the previously administered drug or a drug with similar properties (Preda).
Continued training among physicians, a greater awareness among patients who are prescribed opioids for pain management and the continued efforts of addiction professionals are required in order to move forward in the battle against opioid addiction.
References
Preda, A. M.D. “Opioid Abuse” Medscape; Drugs, Diseases, and Procedures. WebMD LLC. Web. Retrieved from: http://emedicine.medscape.com/article/287790-overview#showall
“Opiate Withdrawal”. MedlinePlus. A.D.A.M. Web. Retrieved from: http://www.nlm.nih.gov/medlineplus/ency/article/000949.htm
“Use, Abuse, Misuse & Disposal of Prescription Pain Medication Clinical Reference”. American College of Preventive Medicine. American College of Preventive Medicine. Web. Retrieved from: http://www.acpm.org/?UseAbuseRxClinRef